The Pooled Cohort Equations: How ASCVD Risk Is Calculated
The PCE were derived from long-term cohort studies — Atherosclerosis Risk in Communities (ARIC), Cardiovascular Health Study (CHS), CARDIA, and the original Framingham Heart Study — encompassing over 25,000 participants followed for 10+ years. The equations use a Cox proportional hazards model with separate coefficients for four population groups (white women, white men, African American women, African American men).
Required Input Variables
| Variable | Range/Options | Why It Matters |
|---|---|---|
| Age | 40–79 years | Strongest risk factor; risk doubles each decade after 55 |
| Sex | Male/Female | Men have higher risk at all ages (until ~80) |
| Race | White/African American/Other | Separate coefficients for race-specific risk |
| Total cholesterol | 130–320 mg/dL | Higher total LDL = more atherosclerotic plaque |
| HDL cholesterol | 20–100 mg/dL | Higher HDL is protective ('good cholesterol') |
| Systolic BP | 90–200 mmHg | Key modifiable risk factor |
| BP treatment | Yes/No | Being treated indicates pre-existing hypertension |
| Diabetes | Yes/No | Doubles cardiovascular risk |
| Current smoker | Yes/No | Doubles risk; reversible benefit after quitting |

Understanding Your ASCVD Risk Score
2018 ACC/AHA Guideline Risk Categories
| 10-Year Risk | Category | Statin Recommendation |
|---|---|---|
| Less than 5% | Low risk | Lifestyle modification; statin generally not recommended |
| 5% to 7.4% | Borderline risk | Risk discussion; statin if risk-enhancing factors present |
| 7.5% to 19.9% | Intermediate risk | Moderate-intensity statin if risk discussion favors therapy |
| 20% or higher | High risk | High-intensity statin strongly recommended |
What the Score Means
A 10-year ASCVD risk of 15% means that 15 out of 100 people with your risk profile will experience a heart attack or stroke within the next 10 years. The 2018 ACC/AHA Blood Cholesterol guideline (Grundy et al., Circulation, 2019) uses this threshold to guide shared decision-making between patient and clinician about statin initiation.
Risk-Enhancing Factors
The 2018 guidelines identify additional factors that, when present, favor statin therapy in borderline or intermediate-risk patients: family history of premature ASCVD (men <55, women <65), persistently elevated LDL-C ≥160 mg/dL, metabolic syndrome, chronic kidney disease, preeclampsia history, South Asian ancestry, elevated hs-CRP (≥2.0 mg/L), Lp(a) ≥50 mg/dL, apoB ≥130 mg/dL, or ankle-brachial index <0.9.
Reducing Your ASCVD Risk: Impact of Lifestyle Changes
Quantified Impact of Risk Factor Modification
| Intervention | Risk Reduction | Source |
|---|---|---|
| Statin therapy (high-intensity) | 25–35% relative reduction | CTT meta-analysis, Lancet 2010 |
| Blood pressure control (to <130/80) | 20–30% relative reduction | SPRINT trial, NEJM 2015 |
| Smoking cessation | 50% reduction within 1 year | Framingham Heart Study |
| Mediterranean diet | 30% reduction | PREDIMED trial, NEJM 2018 |
| Regular exercise (150 min/week) | 20–35% reduction | AHA Scientific Statement 2019 |
| Weight loss (5–10% body weight) | 10–20% reduction | Look AHEAD trial |
| Diabetes control (HbA1c <7%) | 15–25% reduction | UKPDS, Lancet 1998 |
Statins: The Evidence
The Cholesterol Treatment Trialists' (CTT) Collaboration meta-analysis of 170,000+ participants across 27 trials (Lancet 2010) demonstrated that each 38.7 mg/dL (1 mmol/L) reduction in LDL cholesterol with statin therapy reduces major cardiovascular events by 22% and all-cause mortality by 10%. For patients with 10-year ASCVD risk ≥7.5%, statins produce a net benefit — preventing more events than adverse effects caused. The most common side effect, muscle symptoms, occurs in approximately 5–10% of patients (SAMSON trial, NEJM 2022 showed most muscle symptoms are nocebo effect).
Limitations and Accuracy of the Pooled Cohort Equations
Known Calibration Issues
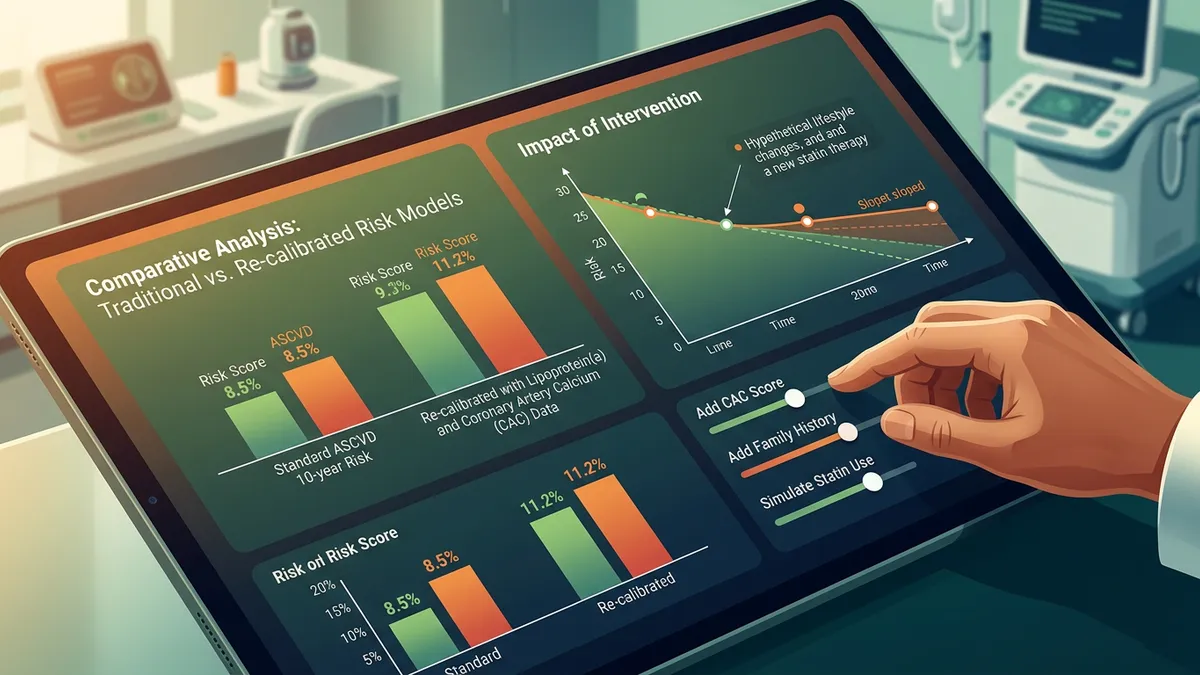
Multiple validation studies have found that the PCE overestimates risk in some populations by 20–60% — particularly in well-educated, higher socioeconomic status populations who have better health behaviors than the original cohort participants. A 2024 JAMA Internal Medicine systematic review confirmed persistent overestimation across 19 external validation cohorts, leading some clinicians to apply a 'recalibration factor' or use coronary artery calcium (CAC) scoring as an adjunct.
Populations Not Well Represented
- Hispanic/Latino populations: The PCE was derived primarily from white and African American cohorts; the MESA study suggests risk may be overestimated in Hispanic populations
- Asian populations: Not included in the derivation cohorts; the QRISK3 (UK) or SCORE2 (European) calculators may be more applicable
- Young adults (<40): The calculator is validated for ages 40–79; lifetime risk assessment is recommended for younger individuals
- Very elderly (>79): Limited data; risk/benefit of statin initiation after 75 is actively debated
Coronary Artery Calcium (CAC) Scoring
For patients at intermediate risk (7.5–19.9%), the 2018 ACC/AHA guidelines recommend CAC scoring (a low-dose CT scan) to further refine risk. A CAC score of 0 reclassifies many patients to low risk (event rate <5% over 10 years), potentially avoiding unnecessary statin therapy. The MESA study (Multi-Ethnic Study of Atherosclerosis) demonstrated that CAC adds significant predictive value beyond the PCE alone.
How Clinicians Use ASCVD Risk Scores in Practice
The Risk Discussion
The 2018 ACC/AHA guidelines emphasize shared decision-making: the ASCVD risk score is a starting point for a clinician-patient discussion, not an automatic prescription trigger. The clinician should explain: the patient's estimated 10-year risk in plain terms, the absolute benefit of statin therapy (number needed to treat, NNT), potential side effects, and the patient's values and preferences. For a patient with 12% 10-year risk, the NNT for 10 years is approximately 30 — meaning 30 patients must take a statin for 10 years to prevent one cardiovascular event.
The 2018 Guideline Treatment Algorithm
- Calculate 10-year ASCVD risk using PCE
- If LDL-C ≥190 mg/dL → High-intensity statin (regardless of risk score)
- If diabetes (age 40–75) → At least moderate-intensity statin
- If 10-year risk ≥20% → High-intensity statin
- If 7.5–19.9% → Clinician-patient risk discussion; consider risk-enhancing factors and CAC
- If 5–7.4% → Risk discussion if risk-enhancing factors present
- If <5% → Emphasis on healthy lifestyle
Beyond Statins: Additional Therapies
For patients with ASCVD risk ≥7.5% not adequately controlled by statins alone, the 2018 guidelines recommend: ezetimibe (lowers LDL an additional 18–25%), PCSK9 inhibitors (evolocumab, alirocumab — lower LDL by 50–60% but cost $5,000–$14,000/year), bempedoic acid (for statin-intolerant patients), and inclisiran (twice-yearly injection, FDA-approved 2021). Aspirin is no longer routinely recommended for primary prevention due to bleeding risk (ASPREE trial, NEJM 2018).
Step-by-Step Instructions
- 1Enter your age (calculator validated for ages 40–79).
- 2Select your sex and race/ethnicity.
- 3Input your latest total cholesterol and HDL cholesterol levels (from a recent blood test).
- 4Enter your systolic blood pressure and whether you're currently on BP medication.
- 5Indicate diabetes status and current smoking status.
- 6View your 10-year ASCVD risk percentage and risk category — discuss results with your healthcare provider.
